It took TV’s ‘Doctor House’, the fictional super-brained ‘Diagnostician’ based on Sherlock Holmes, an hour-long episode to arrive at an endometriosis diagnosis. The patient was theatrically bleeding from her eyeballs and ears. A diagnosis of a more subtle-presenting case of endometriosis it seems, based on this track record, would take at least a whole season.
Endometriosis is a common but still incompletely understood condition that affects around one in ten women, or roughly 190 million women globally, with an average diagnostic delay of seven to ten years that varies by country and health system [1–3]. Current interest in diagnostics is driven by the need to move beyond invasive, late-stage confirmation towards earlier, more objective assessment that supports better clinical decisions.
What is endometriosis?
Endometriosis is a chronic inflammatory condition where tissue similar to the endometrium (the lining of the uterus) grows outside the uterus. Lesions most commonly occur within the pelvis (for example on the ovaries, fallopian tubes and peritoneum) but can also be found outside the pelvis, such as in the gastrointestinal and urinary tracts, abdominal wall, diaphragm and thoracic cavity. In rare cases, endometriosis lesions are found in the lungs, eyes and brain [4–6]. Studies suggest that extra-pelvic disease may, in some cases, reflect dissemination through the bloodstream or lymphatic system [6].
The condition is increasingly understood as a systemic disorder of inflammation and lesions, which can appear in different parts of the body, not just the pelvis or reproductive organs. It is biologically and clinically heterogeneous, with highly variable symptom profiles. Some individuals experience severe, ongoing pelvic pain and heavy menstrual bleeding, while others report fatigue, bowel or bladder symptoms, pain during sexual intercourse, or difficulty becoming pregnant. Symptom severity does not reliably correlate with the extent of disease [7,8].
Endometriosis is also visually and structurally diverse. The tissue can vary significantly in appearance and structure depending on the individual and the stage of the condition. Some lesions are more biologically active, with increased blood flow and inflammation. Others represent more established disease, where ongoing tissue damage and repair have led to scarring. These differences reflect underlying variation in blood supply, immune response, tissue remodelling, and hormone sensitivity, which contribute to the complexity of the condition. Disease stage does not consistently predict pain severity or overall impact [8,9].
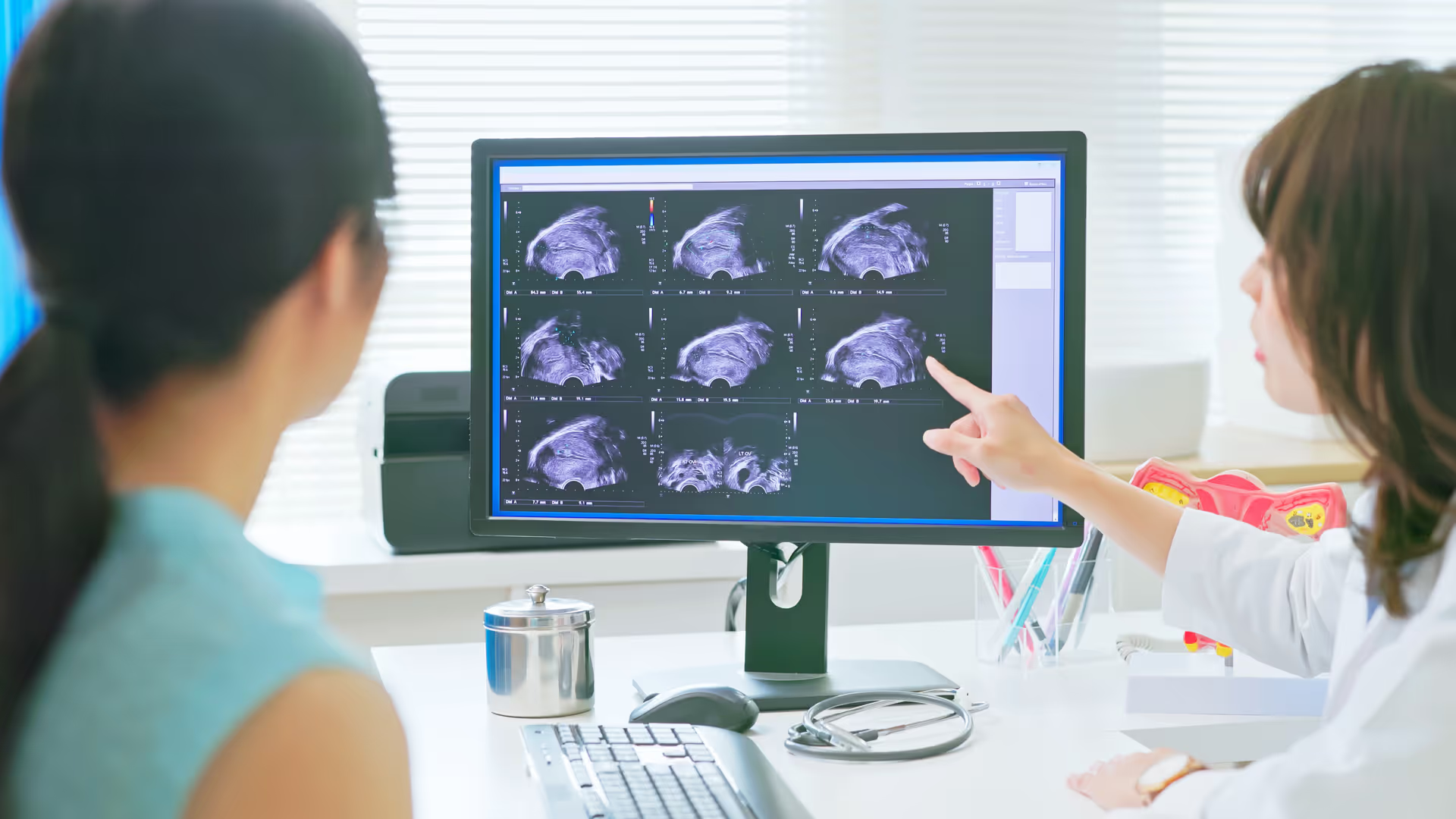
Current diagnostic approaches remain operator-dependent. Specialist transvaginal ultrasound can detect deep infiltrating disease with good sensitivity in experienced hands, but performance varies with expertise, and laparoscopy relies on visual identification of potentially subtle or atypical lesions. Diagnostic delay remains common, and overall disease burden may therefore be underestimated [7,8].
Clinical and economic impact - why is it costing us so much?
When endometriosis affects multiple organs, it can lead to complex, long-lasting symptoms that seriously impact daily life and overall quality of life. Studies in high-income countries show that the annual cost per person is often in the five-figure range. Notably, indirect costs, such as lost productivity and time off work, account for around two-thirds of this total. One study estimated that the average yearly cost per woman affected ranges from Int$16,970 to $20,898, with more than 75% attributable to productivity losses rather than direct medical expenses [10,11]. These findings highlight that endometriosis is not only a medical issue but also a condition with substantial societal and economic consequences.
Data from the US suggest that women with endometriosis have about four times the risk of chronic opioid use and dependence compared with women without the condition, reflecting both the severity of pain and limitations in current treatment options [12]. Delays in diagnosis and prolonged uncertainty are also linked to higher mental health burden and repeated interactions with healthcare services [11]. Treatment is mainly focused on managing symptoms, using pain relief, hormonal therapies, and surgery, but the disease often recurs or persists [5].
Current diagnostic approaches
A definitive diagnosis of endometriosis still typically requires diagnostic laparoscopy, a “keyhole” surgical procedure in which a camera is inserted into the abdomen to directly visualise lesions. In many clinical guidelines, diagnosis is then confirmed by histological analysis demonstrating endometrial-like tissue located outside the uterus [6,13].
Surgical staging systems are available, but they correlate only weakly with symptom severity and patient-reported impact, limiting their value as standalone guides to management. Diagnostic delay arises from varied and often non-specific symptoms, uneven access to specialists, long waiting times for surgery, and differing levels of clinician awareness [3].
Imaging techniques such as transvaginal ultrasound and MRI can detect ovarian endometriomas and many deep infiltrating lesions and are integral to modern diagnostic work-up [4]. However, they are less sensitive for early or superficial peritoneal disease and cannot provide definitive information about tissue type, so negative imaging does not exclude endometriosis. Reliance on invasive procedures also restricts systematic longitudinal monitoring and makes it harder to study natural history and treatment response at scale [2].
This context supports the rationale for developing biomarker-based and multi-modal diagnostic tools that can provide earlier, repeatable and more objective assessments [14].
Research and investment landscape
Historically, endometriosis has received far less research funding than its prevalence and economic impact would suggest [15]. In 2022, the US NIH allocated approximately USD 16 million to endometriosis research, around 0.04% of its total budget [15]. Analyses suggest that, if funding reflected its economic burden, annual NIH investment would need to reach USD 250–450 million [15].
Funding is gradually increasing: by FY2024, NIH allocations had risen to around USD 28 million, and national and regional policies in the US, EU, UK and Australia now explicitly identify endometriosis as a priority within broader women’s health strategies [16].
Emerging diagnostic approaches – what’s next?
Non-invasive and minimally invasive diagnostics are a major research focus in endometriosis, particularly circulating biomarkers and enhanced imaging approaches [16,17]. One notable example is a French next-generation sequencing study that identified a salivary miRNA signature capable of distinguishing women with and without endometriosis, reporting mid-90% sensitivity and near-100% specificity within its cohort [17]. This work has since progressed into clinical translation, with CE-marked saliva-based diagnostics such as Ziwig Endotest now available in parts of Europe.
Beyond saliva-based miRNA profiling, multiple groups are advancing blood-based multi-marker panels, multi-omics signatures, uterine-fluid sampling approaches and AI-assisted imaging tools [18,19]. Collectively, these innovations point toward a diagnostic ecosystem of complementary tools for triage, risk stratification, and longitudinal monitoring, rather than a single universal test [14–16]. However, these approaches still need to be tested in larger and more diverse patient groups, with clearer definition of how and when they should be used in clinical practice, and stronger evidence that they improve outcomes and provide value for healthcare systems [14].
The inflection point for endometriosis diagnostics is becoming clearer. Scientific capability, policy recognition and funding momentum are increasingly aligned. The question is no longer whether non-invasive, objective assessment is achievable, but who will move fastest to convert biological innovation into scalable, regulatory-ready and clinically integrated diagnostics.
About TTP's In Vitro Diagnostics Team
As a diagnostics development consultancy, TTP focuses on combining advances in multiple disciplines, including biology, engineering and data science to enable earlier, less invasive, and more informative evaluation of disease status. TTP’s in vitro diagnostics teams provides end-to-end support, from early feasibility and prototyping through verification, validation and scale-up, partnering with pharmaceutical, diagnostics and Women’s Health companies.
Members of our diagnostics team have long taken an interest in neglected areas of diagnostics related to women’s health.
Reference
[1] World Health Organization. Endometriosis – Fact Sheet. 2025. Available at: https://www.who.int/news-room/fact-sheets/detail/endometriosis
[2] Zhai J, et al. Global, regional, and national burden of endometriosis among women of reproductive age. Lancet Global Health. 2022.
[3] University of York. Endometriosis diagnosis: new research on diagnostic delays. 2024. Available at: https://www.york.ac.uk/news-and-events/news/2024/research/diagnosis-endometriosis-delay/
[4] International Federation of Gynecology and Obstetrics (FIGO). Endometriosis: definition, epidemiology and aetiology. Int J Gynaecol Obstet. 2022.
[5] Nisolle M, Donnez J. Peritoneal endometriosis: pathophysiology and implications for diagnosis and treatment. Eur J Obstet Gynecol Reprod Biol. 1997.
[6] Moradi M, et al. Prevalence and characteristics of endometriosis, including asymptomatic cases. Hum Reprod Update. 2020.
[7] National Institute for Health and Care Excellence (NICE). Endometriosis: diagnosis and management (NG73). London: NICE; 2017 (updated 2024).
[8] Becker CM, Bokor A, Heikinheimo O, et al. ESHRE guideline: endometriosis. Hum Reprod Open. 2022;2022(2):hoac009.
[9] Royal College of Obstetricians and Gynaecologists (RCOG). Endometriosis: Investigation and Management. Green-top Guideline No. 24. London: RCOG.
[10] Rawson JM. The economic burden of endometriosis. J Reprod Med. 2011.
[11] Scottish Government. Endometriosis: Lived experience insight report. 2023.
[12] Tran N, et al. Chronic opioid use and dependence in women with endometriosis. J Pain Res. 2021.
[13] Giudice LC. Clinical practice: Endometriosis. N Engl J Med. 2010;362:2389–2398.
[14] Nisenblat V, et al. Non-invasive biomarkers for the diagnosis of endometriosis: a systematic review and meta-analysis. Hum Reprod Update. 2016.
[15] Zondervan KT, Becker CM, Missmer SA. Endometriosis. N Engl J Med. 2020;382:1244–1256.
[16] NIH Research Portfolio Online Reporting Tools (RePORT). Funding data for endometriosis research. 2024 update.
[17] Bendifallah S, et al. Salivary microRNA signature for diagnosis of endometriosis. Diagnostics. 2022.
[18] Frontiers in Reproductive Health. Emerging non-invasive diagnostic approaches in endometriosis. 2023.
[19] Bendifallah S, et al. Salivary microRNA signature for diagnosis of endometriosis. Diagnostics. 2022;12(7):1644. doi:10.3390/diagnostics12071644